Table of Contents
ToggleIntroduction
In the world of regenerative medicine, Platelet-Rich Plasma (PRP) therapy emerges as a beacon of hope for various conditions that can be helped with this innovative approach.
By unlocking the body’s own healing mechanisms, PRP stands out as a versatile treatment, drawing upon a rich concentration of platelets and growth factors from the patient’s own bloodstream.
We’ll delve into the promise PRP holds, spotlighting its role in addressing an array of medical conditions and setting the stage for a deep dive into the science and stories behind this transformative therapy.
Join us as we explore the conditions that can be helped with PRP, and why it’s captivating researchers and patients alike in the quest for healing.
Definition of PRP (Platelet-Rich Plasma)
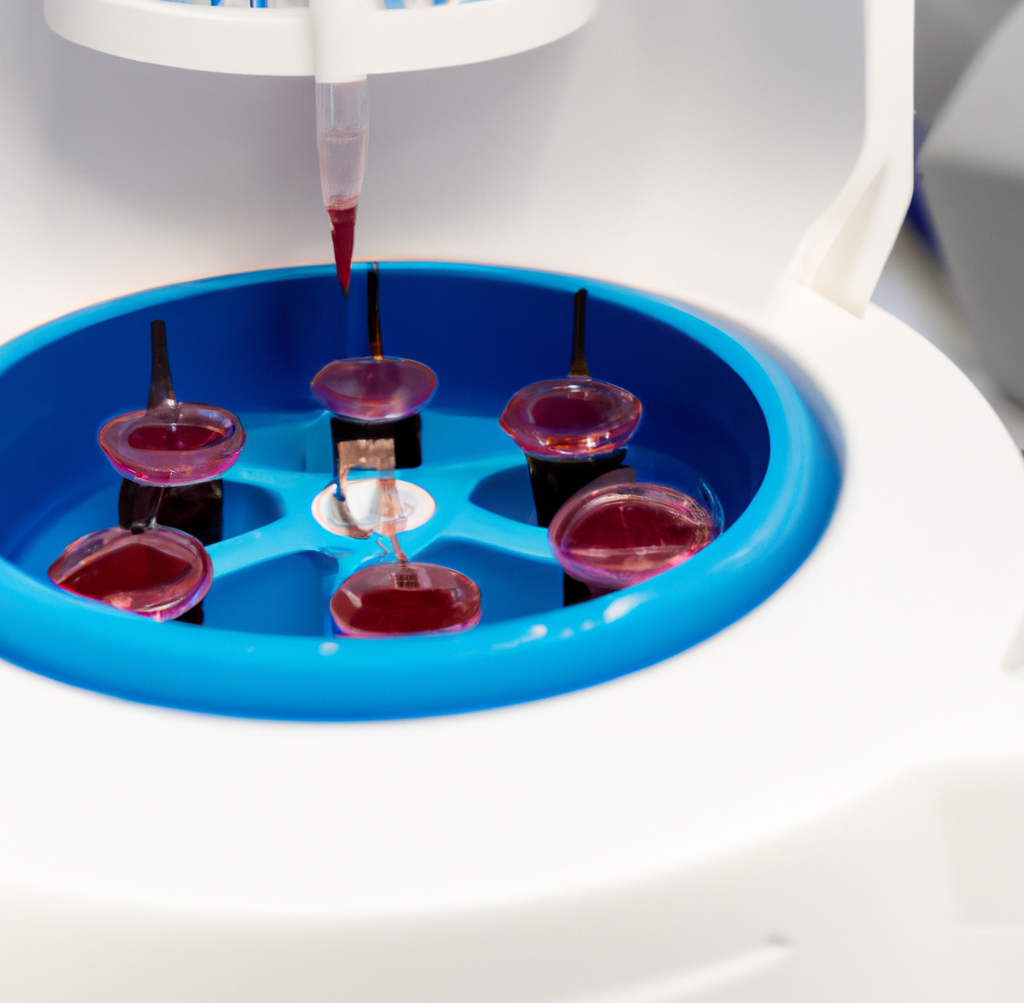
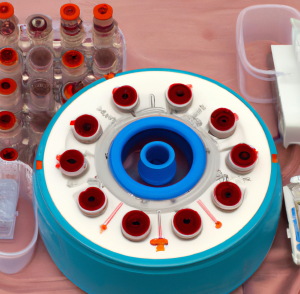
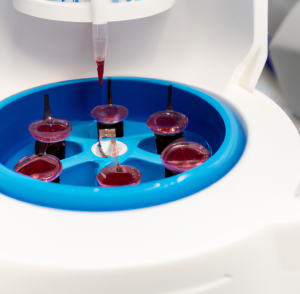
PRP is a concentrated form of plasma obtained by spinning down a patient’s blood sample in a centrifuge device.
The centrifugation process separates the different components within the blood, allowing for a higher concentration of platelets than what is typically found in whole blood.
To put it simply, platelets are small cells involved in clotting and wound healing processes.
They contain numerous growth factors such as transforming growth factor-beta (TGF-β), platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), and insulin-like growth factor-1 (IGF-1).
These growth factors play integral roles in orchestrating tissue repair, stimulating cell proliferation, angiogenesis (formation of new blood vessels), and modulating inflammation.
Therapeutic Potential of PRP
Due to its regenerative properties, PRP has garnered significant attention within orthopedics, dermatology, and other medical specialties.
Its potential applications extend beyond traditional treatment modalities, offering promising results for both acute injuries and chronic conditions.
In the realm of musculoskeletal injuries and disorders, PRP has exhibited notable efficacy in conditions such as tendonitis and tendinosis, ligament sprains and tears, osteoarthritis, and rotator cuff tears.
The growth factors present in PRP aid in tissue repair and regeneration, promoting quicker healing and potentially reducing the need for invasive interventions like surgery.
Moreover, dermatological conditions such as hair loss (androgenetic alopecia), acne scarring, wrinkles, and fine lines have shown improvement with PRP therapy.
The growth factors in PRP stimulate hair follicle regeneration and collagen synthesis, leading to enhanced skin rejuvenation.
Beyond these general applications, PRP therapy has also found niche utilization in dental applications like periodontal disease treatment (gingivitis and periodontitis) or enhancing tooth extraction site healing.
Also, ophthalmological applications for dry eye syndrome treatment or accelerating corneal ulcer healing have been explored.
Musculoskeletal Injuries and Disorders
Tendonitis and Tendinosis
Tendonitis and tendinosis refer to the inflammation and degeneration of a tendon, respectively.
These conditions are often caused by repetitive motions, overuse injuries, or aging.
PRP therapy has emerged as a promising treatment option for tendon-related issues, offering a potential solution for individuals who have struggled with chronic pain and limited mobility.
When PRP is injected into the affected tendon, it stimulates the body’s natural healing process by delivering a concentrated dose of growth factors. T
hese growth factors promote tissue regeneration, increase blood supply to the injured area, and help reduce inflammation.
Studies have shown that PRP injections can lead to significant improvements in pain relief and functional recovery among patients with tendonitis or tendinosis.

Ligament Sprains and Tears
Ligament sprains and tears are common sports-related injuries that can cause significant pain, instability, and functional limitations.
Traditional treatment options for ligament injuries include rest, physical therapy, bracing, or in severe cases, surgical intervention.
However, PRP therapy has emerged as an alternative or complementary treatment modality that shows promising results in promoting ligament repair.
When applied to ligament injuries such as sprains or partial tears, PRP injections facilitate tissue regeneration by triggering the release of growth factors that stimulate collagen production.
Collagen is a crucial component of ligaments responsible for their strength and stability.
By enhancing collagen synthesis through PRP therapy supplements, damaged ligaments can heal more effectively while reducing scar tissue formation.
Moreover, studies have demonstrated that PRP injections can improve pain relief and functional outcomes in patients with chronic ligament injuries who have not responded well to conservative treatments.
The regenerative properties of PRP make it a valuable option for athletes and individuals seeking a faster, less invasive route to recovery.
Osteoarthritis
Osteoarthritis is a degenerative joint disease characterized by the breakdown of cartilage, causing pain, stiffness, and reduced mobility.
While there is no cure for osteoarthritis, treatment focuses on managing symptoms and slowing down its progression.
PRP therapy has emerged as a potential breakthrough in osteoarthritis management, providing hope for patients seeking alternative options to alleviate their symptoms.
PRP injections into arthritic joints help stimulate tissue repair and regeneration by delivering growth factors that promote cartilage restoration.
These growth factors aid in reducing inflammation within the joint and stimulating the production of new cartilage cells.
As a result, this can lead to improved joint function, decreased pain levels, and an overall enhancement in quality of life for individuals suffering from osteoarthritis.
Rotator Cuff Tears
The rotator cuff is a group of muscles and tendons that surround the shoulder joint, providing stability and facilitating movement.
Rotator cuff tears can occur due to trauma or degeneration over time, resulting in pain, weakness, restricted range of motion, and difficulty performing daily activities.
While surgical intervention has been considered the gold standard treatment for severe rotator cuff tears traditionally, PRP therapy offers a less invasive alternative worth exploring.
PRP injections targeted directly into the site of the rotator cuff tear can provide a concentrated dose of growth factors that promote tissue regeneration and healing.
Other Uses for PRP Therapy
Dental Applications
One notable area where PRP has made a significant impact is in periodontal disease treatment.
Gingivitis, which is characterized by inflammation and bleeding of the gums, can be effectively managed with PRP.
The growth factors present in platelet-rich plasma promote tissue regeneration and reduce inflammation, aiding in the recovery process.
Additionally, PRP is beneficial for treating periodontitis, a more severe form of gum disease that can lead to tooth loss if left untreated.
By stimulating tissue repair and accelerating healing, PRP can assist in combating periodontitis and preserving oral health.
Ophthalmological Applications
Dry eye syndrome is a prevalent problem affecting millions of people worldwide due to insufficient tear production or poor tear quality.
Patients report less burning, itching, and redness from dry eyes after using autologous platelet-rich plasma eye drops.
Targeted injections into the ocular surface further reduce these symptoms.
The growth factors within PRP help stimulate tear production and promote ocular surface healing, providing much-needed relief for those suffering from this chronic condition.
Rarely Known Small Details about PRP Therapy
PRP Preparation Techniques
Two main techniques are used in PRP preparation: the Single Spin Technique and the Double Spin Technique.
The Single Spin Technique is a simpler method that involves a single centrifugation process.
The technician draws blood from the patient and then places it in a centrifuge. It spins at a set speed to separate the components by density.
The red blood cells settle at the bottom, followed by a thin layer of white blood cells, and on top, lies the concentrated platelet-rich plasma.
The Double Spin Technique is more complex but results in higher platelet concentrations.
The plasma layer, rich in platelets and white blood cells, undergoes a second centrifugation instead of partial use or disposal.
This additional spin further refines the plasma for its intended applications.
This second round further separates out any remaining red or white blood cells from what becomes highly concentrated PRP.
PRP Injection Methods
A fine needle injects PRP directly into the injured tissue or joints, guided by ultrasound or fluoroscopy. This process is known as the Direct Injection Method.
Consequently, this technique facilitates the precise injection of PRP into damaged tendons, ligaments, or joints to initiate the required healing process.
On the other hand, for certain dermatological conditions, the Topical Application Method is utilized.
Apply PRP on the skin after microneedling or laser treatment to boost absorption and collagen production.
Commonly, practitioners use this technique to treat conditions such as acne scarring, wrinkles, and fine lines.
PRP Side Effects and Risks
Most of these side effects are minor and temporary in nature.
Minor side effects include temporary pain or discomfort at the injection site.
This can be managed with over-the-counter pain relievers if needed.
Some patients may also experience bruising or swelling around the injection site, which typically subsides within a few days.
Although rare, there is a risk of infection at the injection site; however, proper sterilization techniques significantly minimize this possibility.
A Word from HealthyVibe
Let’s wrap this up with some real talk about PRP therapy—it’s the new healing hero in town.
With its slick Single and Double Spin methods, PRP whips up the perfect healing concoction for your body’s needs.
You power up your cells with it, whether you inject it directly into sore spots or apply it on your skin for that glow-up.
More and more people are buzzing about PRP, and it’s not just hype—it’s a game-changer in healing. It offers a natural fix-it route that could sideline the old ways.
Whether you’re healing up from an injury or keeping your skin game strong, PRP might just be your winning play. It’s safe, it’s trending, and it’s the cool new approach to getting better.
FAQ
What is PRP (Platelet-Rich Plasma)?
PRP is a plasma concentrate from a patient’s blood, obtained using a centrifuge. It contains a higher concentration of platelets, responsible for clotting and wound healing, than typical blood.
Why do medical professionals use PRP?
PRP offers therapeutic potential for various conditions. Its growth factors, like TGF-β and PDGF, promote tissue repair and modulate inflammation. It’s popular in orthopedics, dermatology, dentistry, and ophthalmology.
How does PRP benefit musculoskeletal injuries?
PRP can treat tendonitis, tendinosis, ligament sprains, osteoarthritis, and rotator cuff tears. It accelerates healing, reduces inflammation, and sometimes negates the need for surgery.
Are there niche applications for PRP?
Yes, in dentistry, PRP enhances healing post-tooth extraction and helps treat periodontal disease. In ophthalmology, it addresses dry eye syndrome and accelerates corneal ulcer healing.
Are there risks or side effects with PRP therapy?
Generally, PRP is safe. Minor side effects include temporary pain, bruising, or swelling at the injection site. Proper sterilization minimizes infection risks.