Table of Contents
ToggleIntroduction to Scleroderma
Scleroderma is a rare and chronic autoimmune disease that messes with your connective tissues.
This condition causes your body to produce excess collagen, which results in an abnormal thickening and hardening of the skin and other tissues.
This sneaky condition can manifest in various ways, affecting different parts of your body like the skin, blood vessels, muscles, and even internal organs.

Causes and Types of Scleroderma
The exact cause of scleroderma remains a bit mysterious. Researchers suspect it has something to do with a combination of genetic predisposition and environmental triggers.
Localized scleroderma and systemic sclerosis (SSc). Localized scleroderma is like that neighborhood ice cream shop—it stays in one area without causing much trouble elsewhere.
It makes irregular patches on the skin harden up, and linear scleroderma, which can leave a streaky trail of hardened skin.
On the other hand, SSc is like that rock concert that gets out of control—it’s a wild ride affecting not only your skin but also your internal organs.
Scleroderma Patient Symptoms
Living with scleroderma can bring forth a myriad of symptoms that vary from person to person.
The most common symptom is skin tightening, which can affect the hands, face, and other areas of the body.
This tightness may make it challenging to move or flex the affected joints, leading to a sense of stiffness and discomfort.
Individuals with scleroderma often experience Raynaud’s phenomenon, where fingers and toes become numb or change color in response to cold temperatures or stress.
Digestive issues are prevalent among patients and may manifest as difficulty swallowing due to esophageal dysfunction or acid reflux.
Lung complications are another concern in scleroderma cases, resulting in shortness of breath or dry coughs due to scarring of lung tissue.
Scleroderma’s Impact on Body Parts
Scleroderma is a multi-system disease that extends beyond the skin’s involvement.
When esophageal muscles become weakened by scleroderma-related changes, swallowing becomes challenging for patients—sometimes leading to malnutrition or unintentional weight loss.
In terms of pulmonary complications, fibrosis (scarring) can occur within the lung tissues themselves due to inflammation caused by scleroderma.
Scleroderma can also affect the heart muscle itself or cause damage to blood vessels connected to it (known as pulmonary hypertension) which adds additional strain on this vital organ—potentially leading to fatigue, chest pain, or even heart failure.
Conventional Treatment Approaches for Scleroderma
Medications for Symptom Management and Disease Progression
A variety of medications are available, each targeting different aspects of the condition.
One commonly prescribed category of drugs is immunosuppressants.
These medications work by suppressing the overactive immune system response seen in scleroderma patients.
By reducing immune activity, they can help alleviate inflammation and prevent further damage to affected organs.
How Immunosuppressants work
Immunosuppressant drugs used in scleroderma treatment options include methotrexate, mycophenolate mofetil, cyclophosphamide, and azathioprine among others.
These medications act by dampening the immune system’s response which leads to inflammation and fibrosis seen in scleroderma.
Common side effects may include gastrointestinal disturbances such as nausea or diarrhea, increased susceptibility to infections due to reduced immune response, potential for liver toxicity, or bone marrow suppression with long-term use.
Enhancing Blood Flow with Vasodilators
Another class of drugs used in treating scleroderma is vasodilators, which help improve blood flow to the affected areas.
Scleroderma can lead to a narrowing of blood vessels called vasospasms, causing poor circulation and tissue damage.
Vasodilator medications work by relaxing blood vessels and improving blood flow throughout the body.
This can help relieve symptoms such as Raynaud’s phenomenon, which is characterized by cold fingers and toes due to restricted blood flow.
Managing Pain and Inflammation with NSAIDs
Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to manage pain and inflammation associated with scleroderma.
These medications, including ibuprofen or naproxen sodium, work by inhibiting the production of certain enzymes called cyclooxygenases that are involved in the inflammatory response.
By reducing inflammation, NSAIDs can help alleviate joint pain, muscle aches, and stiffness experienced by scleroderma patients.

Emerging Therapies in Scleroderma Treatment
Regenerative Medicine: Stem Cell Transplantation
Stem cells are the building blocks of our bodies, capable of transforming into various specialized cells.
In the case of scleroderma, stem cell transplantation offers a glimmer of hope by replenishing damaged tissues and promoting healing.
In stem cell transplantation, there are two primary approaches: autologous and allogeneic.
Autologous stem cell transplantation harvests and reintroduces a patient’s own stem cells after intensive treatment.
Allogeneic stem cell transplantation uses stem cells from a donor.
Benefits and Risks of Cell Transplantation
Research suggests that this procedure can help reduce skin thickness, improve lung function, alleviate joint pain, and enhance overall quality of life.
By rejuvenating damaged tissues and modulating immune responses, stem cell transplantation offers a ray of hope for those living with scleroderma.
There are some risks and side effects to be aware of though.
The high-dose chemotherapy or radiation used as part of the transplant preparation can weaken the immune system temporarily.
Infections become a concern during this vulnerable period.
There is always a small risk that transplanted stem cells may attack healthy tissues (graft-versus-host disease) in cases where allogeneic transplantations are performed.
Immunotherapy: Targeting Immunity to Stop Disease
Scleroderma is fundamentally an autoimmune disease, where the immune system mistakenly attacks healthy tissues.
Current clinical trials investigating immunomodulatory drugs aim to halt or slow down the progression of scleroderma by modulating specific immune responses responsible for tissue fibrosis and inflammation.
These drugs work by suppressing or modifying specific immune cells or molecules that play a crucial role in driving the disease process.

Recent Immunotherapy Studies Show Promise
Recent studies have shown promising results with drugs such as rituximab, tocilizumab, and abatacept, among others.
These medications target different aspects of the immune system and have demonstrated efficacy in reducing skin fibrosis, improving lung function, relieving joint pain, and enhancing overall patient well-being.
While more research is needed to fully understand these treatments’ long-term effects and establish their optimal use in different subsets of scleroderma patients, they offer a beacon of hope for individuals seeking relief from this challenging condition.
As science progresses further on this front, it brings renewed optimism for those living with scleroderma as they navigate their treatment options.
Alternative Scleroderma Relief Methods
Nutrition’s Impact on Symptom Management
An anti-inflammatory diet is often recommended for scleroderma patients as it focuses on reducing inflammation in the body, which is a key factor in this condition.
This diet encourages consuming foods rich in antioxidants, omega-3 fatty acids, and fiber while minimizing processed foods, refined sugars, and saturated fats.
An anti-inflammatory diet for scleroderma typically includes plenty of fruits and vegetables such as berries, leafy greens, and colorful produce that are packed with vitamins and minerals.
Whole grains like quinoa and brown rice provide essential fiber while lean proteins like fish or legumes offer valuable nutrients.
Incorporating sources of healthy fats like avocados, nuts, or olive oil can further support the body’s inflammatory response.

Foods Triggering Symptoms or Flare-Ups
Every individual with scleroderma may have different triggers based on their body’s response.
Caffeine found in coffee or teas can potentially aggravate gastrointestinal issues commonly experienced by individuals with scleroderma such as acid reflux or heartburn.
Alcohol consumption can also contribute to these digestive problems along with potential interactions between alcohol and medications.
Spicy foods may increase inflammation and cause discomfort for some patients.
High-sodium meals, such as those found in processed or fast foods, can lead to water retention and exacerbate symptoms like swelling or tightness in the skin.
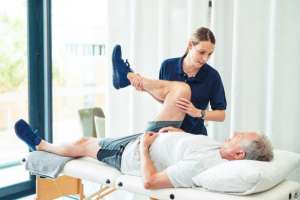
Physical Therapy
A skilled physical therapist can assess the specific needs of each patient and design a tailored exercise program that aims to address joint stiffness, muscle weakness, and range-of-motion limitations often associated with the condition.
Physical therapy for scleroderma may include gentle stretching exercises to improve flexibility, strengthening exercises to build muscle strength, and aerobic activities to enhance cardiovascular health.
These interventions not only promote mobility but also help manage pain and fatigue commonly experienced by patients.
Conclusion
Scleroderma treatment options encompass more than just conventional medications; complementary approaches like dietary changes and physical therapy offer hope for relief from its debilitating symptoms.
By adopting an anti-inflammatory diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats while avoiding triggers such as caffeine or processed foods, individuals with scleroderma can optimize their overall well-being.
Coupled with regular physical therapy sessions tailored to individual needs, it is possible to improve joint mobility, muscle strength, and overall quality of life.









